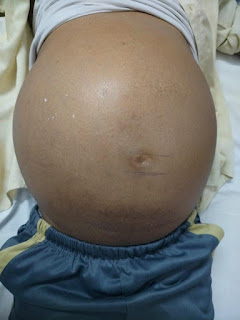
A 45 yr old male came with complaints of abdominal distension ,sob and swelling in both legs since one week
This is an online E-log book to discuss our patient's de-identified health data shared after taking his/her/guardian's signed informed consent. Here we discuss our individual patient's problems through series of inputs from available global online community of experts with an aim to solve those patient's clinical problems with collective current best evidence based inputs.
This E log book also reflects my patient centered online learning portfolio and your valuable comments on comment box is welcome.
I have been given this case to solve in an attempt to understand the topic of " patient clinical data analysis" to develop my competency in reading and comprehending clinical data including history, clinical findings, investigations and come up with diagnosis and treatment plan.
Presenting complaints:
A 45 years old male,resindent of kodakonla mandal,janagam district hotel server by occupantion came with complaints of abdominal distension and shortness of breath and swelling of both lower limbs since 1 week

HOPI:
Patient was asymptomatic,6 years ago and then he developed a minor injury to neck which was not healing and then went for regular checkup and was diagnosed as having diabetes and started on OHA, and 3 years ago he was diagnosed to be having hypertension and started on Tab. Telmisartan 40mg/OD,and was asymptomatic 7 months ago and then in the evening he suddenly became ,unresponsive and irrelevant talk and was taken to hospital and was found to be having hypoglycaemia and was asked to stop OHA,and was found to be having jaundice at that time and was asked to avoid alcohol but he didn’t stopped alcohol consumption.
And 5 months ago,he developed similar complaints and was admitted here and was diagnosed to be having,Acute decomponsated liver disease and was kept on conservative management, a diagnostic and therapeutic tap was done,showing 200cells,lymphocytic predominant cells and High saag and low protein profile and therapeutic Paracentesis was done 1L on day 1
1.75L on day 2 and 1.5L on day 3 and his complaints resolved and was discharged in a hemodynamically stable state,and was normal till 15 days and started developing pedal edema ,abdominal distension and SOB again and came here for further management.
Decreased Apetite and sleep since 2 days.
Chronic alcoholic since 20 years and last binge,30days ago.
Chronic smoker since 30years
Past history:
K/c/o CLD Since 5 months
K/c/o HTN since 2 years
K/c/o DM II since 6 years
Personal history:
Chronic alcoholic consumes 3 quarters/day
Chronic smoker 40 cigarettes/day (since 30 years)
GENERAL PHYSICAL EXAMINATION:
At admission
Patient is drowsy but arousable,
Icterus : present
Clubbing: present
Pedal edema: pitting type
No signs of cyanosis, generalised lymphadenopathy
Bp 140/80mmHg
PR 98bpm
RR 18cpm
Temp Afebrile
Spo2 98% on RA
SYSTEMIC EXAMINATION:
CARDIOVASCULAR SYSTEM:
S1 AND S2 HEARD. NO MURMURS
RESPIRATORY SYSTEM: BAE PRESENT. NVBS HEARD
CENTRAL NERVOUS SYSTEM:
Patient is drowsy and arousable
Speech normal
No signs of meningeal irritation
P/A
Distended,and
umbilicus everted
Dilated veins present over the lower aspect of abdomen
And shifting dullness positive and fluid thrill negative.
Abdominal girth 124cms
Genitals examination:
Scrotal swelling present
Ascitic fluid diagnostic tap was done showing High saag and low protein (0.8)and Total cells 300,lymphocytic predominant (80%)
Therapeutic tap of 1 litre was done
Therapeutic paracentesis done on 28/02/2023 of 2 litres
INVESTIGATIONS:
ULTRASOUND:
IMPRESSION:
1. Heteroechoeic echotexture with surface irregularity of liver , correlate with LFT
2. gross ascites
3. PV shows to and fro flow
4. B/l raised echogenecity of kidneys
ECG:
CHEST X RAY
Apraxic charting:
On 27/02/2023
APTT: 35 SEC
BLEEDING TIME: 2MIN 30 SEC
CLOTTING TIME: 5 MIN
BLOOD GROUPING: O POSITIVE
BLOOD UREA: 36 mg/dl
SERUM CREATININE: 1.2 mg/dl
PROTHROMBIN TIME: 18 sec
INR: 1.33
HCV: NEGATIVE
HBSAG: NEGATIVE
HIV : NEGATIVE
ON 28/02/2023
FBS: 103 mg/dl
SAAG:
SERUM ALBUMIN: 2.2 gm/dl
ASCITIC ALBUMIN: 0.3 gm/dl
SAAG: 1.9
ASCITIC FLUID PROTEIN : 0.8 g/dl
ASCITIC FLUID SUGAR: 151 mg/dl
ASCITIC FLUID AMYLASE: 40.6 IU/L
ASCITIC FLUID LDH: 56.6 IU/L
ASCITIC FLUID ADA: 24 U/L
2D ECHOCARDIOGRAPHY:
No RWMA, MILD LVH (+) (1.2cms)
MODERATE TR+; PAH TRIVIAL AR+; NO MR
SCLEROTIC AV, NO AS/MS
EF: 62. RVSP= 42+10= 52 MM HG
GOOD LV SYSTOLIC FUNCTION
NO DIASTOLIC DYSFUNCTION
MINIMAL PE(+)
IVC SIZE (1.25CMS) COLLAPSING
MILD DILATED R.A/R.V
On 01/03/2023
Blood urea: 16 mg/dl
Serum creatinine: 1.1 mg/dl
Serum Na+ 137 mEq/L
Serum K+ 4.0 mEq/L
Serum Cl- 105 mmol/L
Serum Ca+2 1.05 mmol/l
Diagnosis:
ACUTE DECOMPENSATED ALCOHOLIC LIVER DISEASE
WITH ASCITIS (MODERATE)
WITH GRADE I HEPATIC ENCEPHALOPATHY
WITH ANEMIA(MACROCYTIC)
WITH K/C/O DM 6 YEARS AND HTN 3 YEARS
TREATMENT:
1. INJ. LASIX 60 mg IV/BD
2. INJ. CEFTRIAXONE 2 GM IV/BD
3. INJ. VITAMIN K 10 mg IV/OD
4. FLUID RESTRICTION less than 1.5 litres/day
5. SALT RESTRICTION less than 2 gm/day
6. INJ. PAN 40 mg IV/PD
7. TAB. ALDACTONE 50mg PO/OD
8. TAB. TELMISARTAN 40 mg PO/OD
9. TAB. RIFAGUT 550 mg PO/BD
10. TAB. UDILIV 300 mg PO/OD
11. SYRUP. HEPAMERZ 15 ml PO/TID
12. O2 inhalation
13. Vitals monitoring
14. Abdominal girth monitoring
15. Grbs monitoring
16. SYRUP. LACTULOSE 30 ml PO/TID